Lesson 1
Lack of response from a provider to your dispute does not indicate that your dispute is off track or will be unsuccessful.
There are several reasons providers do not respond to Letters of Dispute. Many providers, especially large health systems and collections agencies, use automated systems and impersonal processes designed to bill and collect from patients, with limited attention to addressing patients’ questions and concerns about these bills. Alternatively, a provider may intentionally disregard a Letter of Dispute because it thinks there is a chance that the patient will pay the bill out of frustration or fear, and the provider prioritizes bringing money in through continued billing over giving time and attention to a patient’s challenge to a medical bill.
A customer understandably may have concerns if the provider has not responded to a Letter of Dispute, and may assume that a lack of response means the dispute is not successful. However, a lack of response from a provider does not help the provider’s position in a dispute. Your Letter of Dispute formally notified the provider, and created a written record, that you are disputing the medical bill, and detailed the reasons for the dispute. The letter further informed the provider that it has 30 days to respond by addressing your concerns and requests, and that you do not intend to pay the Medical Bill until those concerns and requests are resolved to your reasonable satisfaction. The Letter of Dispute is not a magic wand that forces a provider to respond to it (see What a Letter of Dispute Can and Cannot Do), but it is the primary and most effective tool for you to fight for fair treatment. That is an important reason not to abandon the Letter of Dispute, or the dispute itself, simply because the provider is not responding.
Lesson 2
The patient disputing an unpaid medical bill has significant leverage against the billing provider, even if the provider is not responding to a letter of dispute.
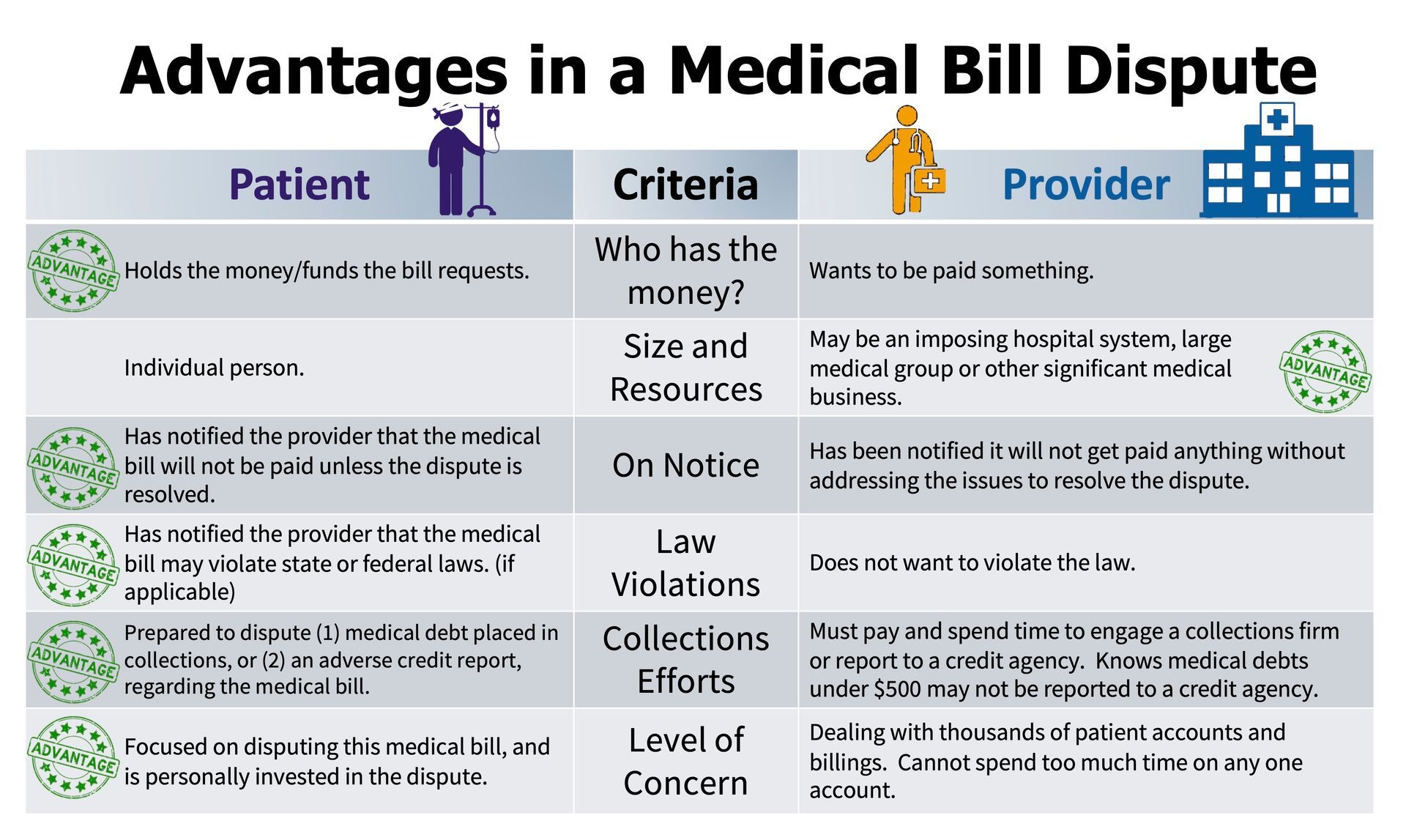
Remember that you are in charge of your dispute, and you have leverage. Consider the circumstances between a patient disputing a bill and the provider issuing the bill.
When viewed through this perspective, the patient has far more control and power in the dispute of the medical bill than the provider, even if the provider is a large hospital system or medical group. The longer the dispute continues, the longer the provider is not receiving any payment, and likely thinks its chances of collecting future payment is shrinking.
Lesson 3
Patience and persistence are essential to a successful dispute.
You are following a plan to challenge your medical bill. A key in that plan is for your Letter of Dispute to put the provider on notice that you require thoughtful responses to questions and concerns about the bill to resolve the dispute.
Seeking fairness in medical billing can mean standing up to unfair medical bills, and not giving in to continued collection efforts even after your challenge in underway and the provider has your Letter of Dispute. Don’t let a provider’s disregard of your Letter of Dispute be a reason for you to abandon your plan to challenge the medical bill. Each time the provider or a collections agency tries to collect from you on the medical bill, you should inform them that:
· You have sent a formal Letter of Dispute on the medical bill.
· Any payment from you is contingent on resolving that dispute.
· The dispute can only be resolved by the provider responding to the letter of dispute, and that the provider should not expect any payment from you until the provider addresses your Letter of Dispute.
The most effective way to respond to phone calls, letters and other attempts to collect on a disputed medical bill is to refer the provider or collections agency back to your Letter of Dispute. Patient Fairness will mail a copy of your Letter of Dispute in response to collections efforts on request, or a customer may download and send a copy himself or herself. This keeps the provider and its agents on notice that the bill is under dispute. Do this consistently each time you are contacted.
Lesson 4
Winning a medical bill dispute by default is still winning a medical bill dispute.
It is more common that a provider stops billing and collection efforts on a disputed medical bill than for the provider to give notice or agree in writing to forgive or rescind the medical bill. That means a patient may not realize that his or her dispute was successful until he or she realizes that he or she is no longer receiving bills anymore.
In this fashion, many successful medical bill disputes end quietly (no more bills) rather than a bang (the provider rescinds, apologizes for, or signs a settlement agreement about the medical bill). The outcome is just as favorable to the patient (the bill goes away), but can be less recognized because not receiving a bill is less apparent than an express concession from the provider.
Because providers frequently end collections efforts on bills without any notice, patients who assume that a provider’s lack of communication can be frightened into paying a bill that the provider would have, or already has, been written off. Waiting out a provider on a dispute can be a patient’s best strategy for a successful dispute.
If a customer has not seen activity for a month or more from a provider or other party related to the dispute or collection of the medical bill, Patient Fairness will offer to issue a follow-up letter about the dispute to the provider. After two months of inactivity from a provider, Patient Fairness will offer to issue a letter to the provider that the customer considers the bill to be invalid given the provider’s failure to address the dispute, and to tentatively close the case as resolved in the customer’s favor. After 12 subsequent months of inactivity from a provider, Patient Fairness will offer to issue a letter to the provider that the customer considers the disputed bill to be forgiven, with nothing owed by the customer, and to permanently close the case as resolved in the customer’s favor.
Lesson 5
You can defend against Collections and Credit Reporting.
You do not need to panic over threats of placing your bill in collections or making adverse reports to credit agencies. Collections and credit reporting may not be as concerning as you think, and Patient Fairness offers tools and services to help you address such tactics by providers.
Sending a medical bill to collections simply means that a provider is going to use a third party, a debt collector or collections agency, to seek payment from you on the bill. A debt collector may contact you more frequently and through new channels, like phone calls, beyond what the provider used in its billing. However, you have important rights under federal and state laws to protect you against unfair debt collection practices. See the article
Medical Debt Collections for more information. Sending a medical bill to collections is not the same as submitting an adverse credit reporting, but a bill collector may make an adverse credit report.
Most disputed medical bills are not reported to credit agencies. By law, medical bills below $500 cannot be reported. Some states, medical bills of any size cannot be reported. See the article
Credit Reporting and Medical Debt for more information.
If you do see a medical bill debt reported to one of the major credit agencies then Patient Fairness can help you dispute the credit report. You can use the documentation from your Letter of Dispute as the basis for the credit report dispute. The debt will be removed from your credit report if you are successful.
Conclusion
Don’t let a provider’s lack of response to your dispute or threats of collection and credit reporting bully you into dropping a dispute necessary for you to be treated fairly.
Patients are not at the mercy of providers that do not respond to, or cooperate with, medical bill disputes. Contrary to what many expect, the patient holds a position of significant strength, one which can give him or her the advantage in a dispute even if the provider is not responsive. Provider threats of adverse credit reporting and collections are not reasons in themselves for a patient to abandon a legitimate dispute.
You may decide to pay a disputed medical bill after understanding better the provider’s perspective and your rights and protections. However, intimidation by the provider typically does not help this understanding. An earnest response from the provider to your Letter of Dispute is normally necessary for such understanding.